Why do many of us experience a gradual or suddenly increasing reactions to not just histamine, but foods on pretty much all the lists (salicylates, oxalates, fructose etc).
Does going on a strict low histamine diet make you more sensitive to other foods? Are we on the wrong track?
Yes and no.
One of the concerns immunologist and author Dr. Janice Joneja shared in my interview with her is the fear of a rebound effect of antihistamines, because the body needs a certain amount of histamine to keep us going (to keep us awake, regulate hormones, jump start the healing process and much more). The idea being that if we mess with our histamine, the body may produce more in order to keep these processes running smoothly, or it just may do so when the antihistamine is withdrawn or wears off. I experienced this in spades myself when weaning myself off the xanax I was addicted to for over a decade (many thanks to the giant pez dispenser/shrink who handed out a never ending supply, assuaging my fears thus: “Don’t worry Yasmina, these .25mg are really basically baby xanax). The surges of anxiety and adrenaline I deal with as the dose declined was way out of proportion to how I would feel just a few months later once my body re-stabilised (like I was reborn!). When weaning myself of my mega dose of antihistamines I experienced the worst symptoms of my life. Even worse than xanax. A rash on my hands and feet and agonising blisters in my throat – symptoms resembling hand foot and mouth disease!
All this information made me question if it’s also possible that strangling the body’s supply of fresh histamine from food sources may in fact cause the body’s mast cells, which safely house histamine and other inflammatory compounds till needed, to break open, dumping histamine (along with many other inflammatory molecules into the bloodstream) to make up for the shortfall?
CLICK HERE TO LEARN HOW EASY IT IS TO CREATE YOUR OWN HISTAMINE BALANCED DIET AND HEALING PLAN.
To be honest I don’t have the answer to this. If I did you better believe that (like the rest of my writing) it would have the hell referenced out of it. Sadly none of the mast cell doctors I’ve asked this of have the answer either. One day hopefully we’ll get someone to take the issue of diet seriously enough to ask these questions. Till then, I can share my experiences and those of others, and maybe give you a little something to think about if you’re suddenly thinking you’re reacting to salicylates, fructose, oxalates et al.
What I’ve found is pretty simple: if you eat less of something, you’re gonna have to eat more of something else to make up for it. So cutting out histamine might mean an increase in salicylate consumption.
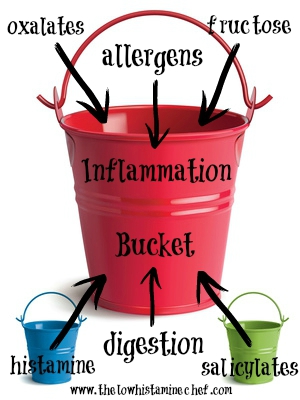
Which brings us to the inflammation bucket, which I have blogged about in the past, but now I’m going to get into it in more detail, along with sharing the nifty little graphic I put together for you above.
In much the same way that I find many of us acquire an alarming number of separate medical conditions that are really just naming symptoms of inflammation without getting to the root cause, I made the mistake early on of believing I had separate issues with: histamine, fructose malabsorption, salicylate intolerance, oxalates and mast cell activation.
Since then I’ve realised that I and a great many of the readers I have spoken with in consults, who email me, and those in my Facebook groups (just search FB for histamine intolerance), generally have sensitive bodies/stomachs. I’m seeing more and more that rather than going totally gonzo on a crazy strict never ending elimination diet and subsisting on meal replacement shakes, or super strict paleo, SCD, autoimmune paleo, it pays to just be a little more mellow and try to maintain a healthy, balanced diet.
How I see things:
Contained within my body is a bucket. Because I have struggled with inflammation in the past, I’ll call it the inflammation bucket.
Within this bucket live lots of other little buckets called: histamine, salicylates, oxalates and fructose (for starters). These little buckets start to fill up as we eat. Eventually, if we fill them enough, they spill over into the bigger bucket, which I see as balanced on a see saw, which then tips to one side, spilling, causing an inflammatory reaction. In the past I simply attributed this to histamine. But finally I realised that eating too much of anything, or just eatbiijsing it too many days in a row without allowing the bucket to empty, was causing the bucket to spill over.
So it’s not that all the little buckets need to spill over, it just takes one, the salicylate bucket for example, to rock the boat.
What are some of the smaller buckets?
Digestion: the digestive process requires histamine to power it and is essentially an inflammatory one [1]. This may be why I have experienced immense relief since giving up snacking. As Dr. Fuhrman covers in his book Eat to Live, if you’re always eating, you’re always releasing inflammation into the body.
Allergens: if you have an undiagnosed allergy it could definitely affect overall inflammation levels. Dr. Theoharides covers this in many of his very informative mast cell charts. Allergens can trigger mast cells (and others), where histamine lives in the body, to dump histamine and other inflammation into the body. I also found that highly allergenic foods, whether on lists as high histamine or not (things like soy sauce, peanuts, corn, yeast), to be major triggers. That one really puzzled me for a long time.
Stress: according to NIH funded mast cell researcher Dr. Theoharides, stress is one of the major mast cell and histamine triggers [2]. Stress, all on its lonesome, can fill me up faster than a media hungry Kardashian on the ALS bucket challenge. I had a major stress last week and my body had a full on meltdown. Total system shutdown, nothing to do with food or inflammation. In my world, stress is the number one trigger, which is why I have spent a considerable chunk of the last few years engaged in daily meditation and yoga.
Other amines and food compounds: histamine is an amine. Many elimination diets advocate chucking as many of these as possible out of your diet. I found balancing them to be a better approach for me, but we’re all different. Salicylic acid is a plant hormone that is also part of its defence mechanism [3]. Oxalic acid is also found in plants and has been found to irritate the bladder and possibly cause kidney stones [4]. Some folks are sensitive to both, even in small amounts.
I’ll be sharing 90 minutes of the best tips I’ve learned over the last five years researching and applying histamine intolerance and mast cell activation techniques to my own life in an online workshop taking place at 10am LA / 1pm New York / 7pm Paris time on Saturday April 23rd. There’ll be a recording of the event available to you as many times as you’d care to watch for seven days afterwards. Check out the event post here.
Emptying the bucket
Avoidance of allergens: based on IgE testing or that recommended by your doctor.
Antihistamine and anti-inflammatory rich diet: I have found that the best way to empty my bucket, or prevent it from filling up in the first place, is eating large amounts of healing, high nutrient foods that are high in antihistamine and anti-inflammatory compounds. Things like the bioflavonoids quercetin, rutin and luteolin, which have been shown to act as mast cell stabilisers and antihistamines [5]. You’ll find plenty of information in the Anti-Cookbook and Man Food. Because of this I now call my approach the histamine-balanced diet, rather than a low histamine one. I am now able to eat most high histamine foods, as long as I balance them with antihistamine and anti-inflammatory ingredients. As an example: half a sliced avocado, served with DAO boosting olive oil, antihistamine and anti-inflammatory cilantro, basil, thyme dressing, on a bed of anti-inflammatory vitamin k rich mesclun greens, paired with an antihistamine and anti-inflammatory green smoothie or juice.
Meditation and yoga: meditation specifically switches off the genes involved in mast cell disorders [6] and yoga has potent anti-inflammatory benefits [7]. I have found that lowering stress/anxiety levels meant I could eat more, lots more, of whatever I wanted (but I only want super healthy foods now anyway!).
Supplements: quercetin, rutin and luteolin can be found in supplements, including Neuroprotek, developed by leading mast cell researcher Dr. Theoharides at Tufts [8]. Nigella sativa meanwhile possesses significant antihistamine benefits [9]. Research has also shown holy basil and olive leaf to be mast cell stabilisers and antihistamine, at least in studies [10]. This doesn’t always translate to human beings. The Anti-cookbook is made up entirely of antihistamine and anti-inflammatory foods, as is Man Food.
No/less snacking: keeping my meal times limited has been a huge help, as has drinking smoothies, salads in a glass and eating lots of soups – possibly because of less stress on stomach enzymes, again according to Dr. Fuhrman in Eat to Live. Don’t miss my post on an exciting new fasting style that may help us slough off faulty mast cells and replace them with new ones.
You can read more about the inflammation bucket in this post.
Please always remember to check with a doctor before trying anything new. I am not a medical professional and as such can only share what has worked for me, and what worked for me may not for others.
Please remember, even antihistamine and anti-inflammatory foods can hurt us, please always exercise caution and consult a medical practitioner before adding new foods.
———REFERENCES——-
[1] https://healinghistamine.com/wondering-why-you-react-to-everything-you-eat/
[2] http://www.mastcellmaster.com
[3] https://en.wikipedia.org/wiki/Salicylic_acid
[4] http://www.drweil.com/drw/u/QAA400344/Avoid-Vegetables-with-Oxalic-Acid.html
[5] The Anti-Cookbook. 2012, Yasmina Ykelenstam.
[6] https://healinghistamine.com/meditation-antihistamine-mast-cell-stabiliser-epigenetic-superstar/
[7] https://healinghistamine.com/fight-histamine-induced-inflammation-yoga/
[8] http://www.mastcellmaster.com
[9] https://healinghistamine.com/plant-seeds-treat-nasal-allergies-better-than-steroid-spray/
[10] The Anti-Cookbook. 2012, Yasmina Ykelenstam.













